Finding lung cancer early can be the difference between a complex surgery and a curative treatment. For a long time, we didn't have a reliable way to catch these tumors before they caused symptoms, but that changed with the introduction of lung cancer screening. While the idea of a "scan" can feel intimidating, the goal is simple: find the problem while it's small enough to fix.
If you have a history of smoking, you might be wondering if you qualify for this preventive care or if the radiation risks outweigh the benefits. With updated guidelines from the U.S. Preventive Services Task Force (USPSTF), millions more people now qualify for these scans than they did just a few years ago. Here is a direct look at how the process works, who needs it, and what you should actually expect during your appointment.
Key Takeaways for High-Risk Smokers
- Who qualifies: Adults aged 50-80 who smoke now or quit within the last 15 years, with at least a 20 pack-year history.
- The Method: A Low-Dose CT (LDCT) scan is used, which delivers significantly less radiation than a standard CT.
- The Benefit: Research shows a 20% reduction in lung cancer deaths for high-risk individuals who get screened.
- The Trade-off: There is a risk of "false positives," where a spot is found that isn't actually cancer.
Who Should Actually Get Screened?
Not everyone who has smoked needs a scan. The medical community uses a specific set of criteria to identify people whose risk is high enough to justify the procedure. USPSTF is the U.S. Preventive Services Task Force, an independent panel of national experts who make evidence-based recommendations about clinical preventive services. Their 2021 update expanded the net to save more lives.
To see if you fit the criteria, you need to look at three factors: age, smoking status, and your "pack-year" history. You are generally eligible if you meet all the following:
- Age: You are between 50 and 80 years old.
- Smoking Status: You currently smoke or you quit smoking within the last 15 years.
- Smoking History: You have a 20 pack-year history or more.
If you're confused about "pack-years," it's a simple math problem. One pack-year is smoking one pack (20 cigarettes) a day for one year. If you smoked one pack a day for 20 years, that's 20 pack-years. If you smoked two packs a day for 10 years, that's also 20 pack-years. Why does this matter? Because it gives doctors a concrete measure of how much your lungs have been exposed to carcinogens over time.
What Happens During a Low-Dose CT Scan?
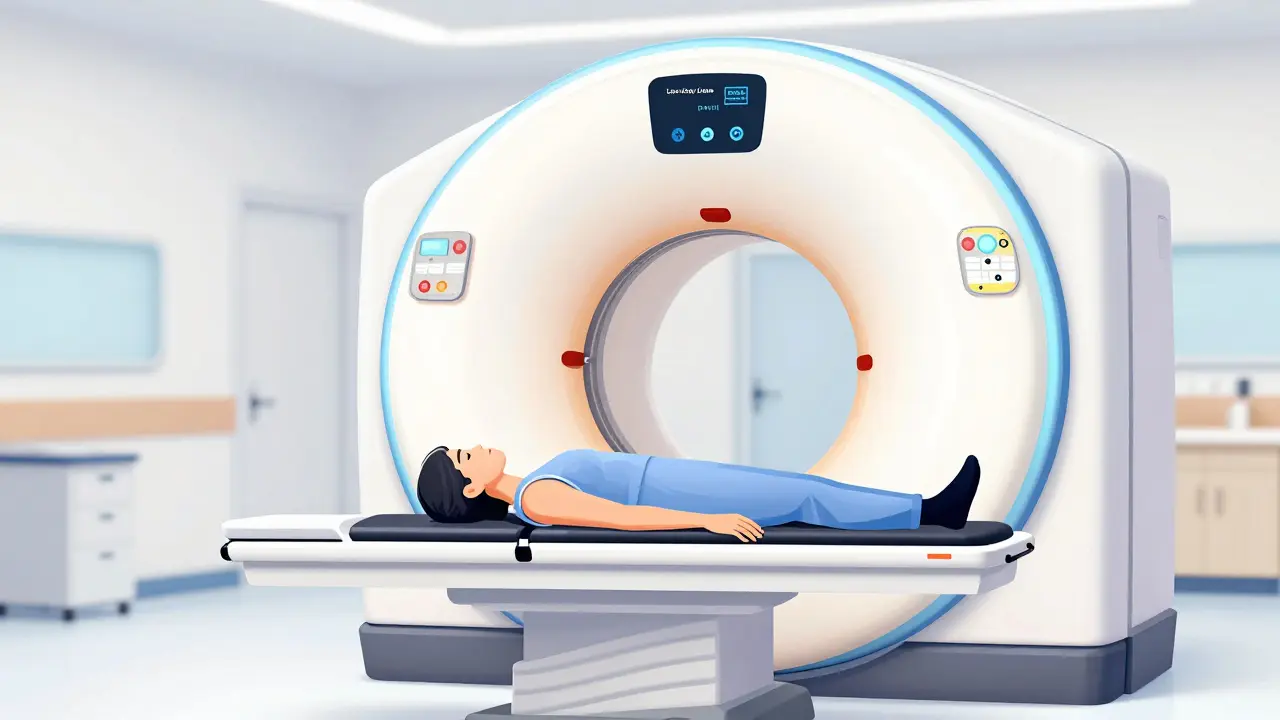
Many people imagine a long, invasive process, but a Low-Dose CT (LDCT) is a specialized computed tomography scan that uses a lower dose of X-rays to create detailed cross-sectional images of the lungs is surprisingly quick. You simply lie on a table and slide through a doughnut-shaped machine. The whole thing usually takes less than 10 minutes.
The "low-dose" part is critical. A standard CT scan might deliver 7-8 millisieverts of radiation, but an LDCT delivers about 1.5 millisieverts. This allows doctors to see tiny nodules (small spots) in the lungs without exposing you to excessive radiation every year.
| Feature | Standard CT Scan | Low-Dose CT (LDCT) |
|---|---|---|
| Radiation Dose | ~7-8 millisieverts | ~1.5 millisieverts |
| Primary Purpose | Diagnosing known symptoms | Screening asymptomatic high-risk people |
| Detail Level | Very High | High (optimized for lung tissue) |
| Frequency | As needed | Typically annual |
The Pros and Cons: Is It Worth It?
No medical procedure is without a downside. The primary goal of LDCT is a reduction in mortality. The National Lung Screening Trial (NLST) proved that this approach could cut lung cancer deaths by 20% compared to traditional chest X-rays, which are far less effective at finding early tumors.
However, the biggest challenge is the "false positive." In the NLST, about 13.9% of screenings per round resulted in a false positive. This means the scan found a spot that looked like cancer, but after further testing-like a biopsy or a follow-up scan-it turned out to be a harmless scar or a benign cyst. This can lead to significant anxiety and unnecessary medical procedures.
There is also the issue of overdiagnosis. Some tumors grow so slowly that they would never have caused a problem in the patient's lifetime. Finding them might lead to surgeries that the patient didn't actually need. Because of this, doctors insist on a "shared decision-making" visit before the first scan to ensure you understand these risks.
Understanding Your Results: The Lung-RADS System
When your scan is finished, the radiologist doesn't just say "it's fine" or "there's a problem." They use a standardized language called Lung-RADS is the Lung Imaging Reporting and Data System, which categorizes CT findings to determine the next clinical step . This ensures that whether you are in New York or California, your results are interpreted the same way.
The categories generally range from 1 to 4:
- Category 1: Negative. No nodules found. You'll likely just come back in a year.
- Category 2: Benign appearance. A small spot was found, but it doesn't look like cancer. Usually results in annual screening.
- Category 3: Probably benign. The spot requires a shorter follow-up (maybe 6 months) to see if it grows.
- Category 4: Suspicious. The spot has characteristics of cancer. This usually leads to immediate diagnostic workups, like a PET scan or a biopsy.
Practical Steps for Getting Started
If you think you qualify, the process isn't as simple as just booking an appointment. Because of the risks of overdiagnosis, insurance providers-including Medicare is the federal health insurance program for people 65 or older and certain younger people with disabilities -often require a documented discussion with your doctor first.
Here is the typical workflow you'll experience:
- The Eligibility Check: Your doctor calculates your pack-years and checks your age.
- The Shared Decision Visit: You spend 20-30 minutes discussing the 20% mortality benefit versus the 13.9% false-positive risk.
- The Scan: You visit an ACR-accredited center (American College of Radiology) to ensure the equipment and staff meet national quality standards.
- The Result: You receive a Lung-RADS score and a plan for the next 6 to 12 months.
If you have trouble finding a facility, remember that not every imaging center is accredited for lung screening. Many people have to travel further than expected to find a center that participates in the required national registry.
The Future of Screening: AI and Risk Models
We are moving away from the "one size fits all" pack-year calculation. New tools like the PLCOm2012 model are starting to look at other factors, such as family history, education level, and current respiratory symptoms, to better predict who is actually at risk.
Even more exciting is the integration of Artificial Intelligence. The FDA has already cleared AI software (like LungAssist) that helps radiologists spot nodules more accurately. In some trials, this technology has reduced false positives by over 15%, meaning fewer people will have to go through the stress of a biopsy for a benign spot.
When should I stop getting screened?
Guidelines suggest stopping LDCT screening if you have successfully quit smoking for 15 consecutive years. Additionally, if you develop a health condition that significantly limits your life expectancy (usually less than 10-15 years) or if you are no longer healthy enough to undergo lung surgery if cancer were found, the scans may no longer be beneficial.
Does Medicare cover the screening?
Yes, Medicare covers annual screenings for adults aged 50-77 who meet the smoking history requirements. Note that their age cap is slightly lower than the USPSTF recommendation of 80. You must have a shared decision-making visit with your provider first for the claim to be approved.
What if the scan finds a "nodule"? Does that mean I have cancer?
Not necessarily. Many nodules are benign (non-cancerous) scars from old infections or small cysts. This is why the Lung-RADS system exists-to categorize the nodule's appearance. If it's Category 2, it's likely harmless. If it's Category 4, further testing is needed to confirm whether it is malignant.
Can't I just get a chest X-ray instead?
A chest X-ray is not a substitute for LDCT. X-rays often miss small tumors that are hidden behind the heart or ribs. The NLST study explicitly showed that LDCT was 20% more effective at reducing deaths than X-rays because it can find cancer at Stage 1, when it is most treatable.
How often do I need to go back for a scan?
For most people with a negative or benign result, the scan is done once every year. However, if a "probably benign" nodule is found (Lung-RADS 3), your doctor might ask you to come back in 3 or 6 months to see if the spot has changed in size or shape.
Next Steps and Troubleshooting
If you realize you meet the criteria but your doctor hasn't mentioned screening, don't wait. Many primary care providers are simply unaware of the updated 2021 guidelines. Bring up the 20 pack-year and age 50-80 criteria during your next visit.
For those in rural areas, finding an ACR-accredited facility can be a challenge. If your local hospital doesn't offer LDCT, check the American College of Radiology's directory of accredited centers. It may be worth a longer drive once a year to ensure you are being screened at a facility that follows the strict national protocols for accuracy.






Carol Yang
April 26, 2026 AT 07:21Glad to see the guidelines expanded. Definitely feels like a win for people who managed to quit but still have that lingering worry about their lungs.
Brittney Prince
April 28, 2026 AT 05:36Typical. They just expand the 'net' to get more people into the system. All this talk about 'low-dose' but we all know how radiation works and how these big labs make money off 'follow-up scans' for every little speck of dust they find. Just more ways to keep us scared and paying.
Vijay AGarwal
April 29, 2026 AT 23:50Listen, the difference between a chest X-ray and an LDCT is absolutely night and day! It is an absolute tragedy that people still think an X-ray is enough. We are talking about catching a killer while it's still small enough to be sliced out of your body! If you're in the risk group, not doing this is practically playing Russian Roulette with your own chest!
Sharyl Foster
April 30, 2026 AT 16:44Actually, the 'shared decision' part is usually just a formality. Most doctors just want to check a box for the insurance company so they can bill the visit. Plus, the anxiety from a Lung-RADS 3 result is often worse than the actual risk of a slow-growing tumor.
Michael Deane
May 1, 2026 AT 19:53Only in America do we have the best medical tech and the most complicated insurance nightmares to actually get it, but hey, that's why we lead the world in innovation while other countries are still using outdated gear from the eighties, so I'll take the paperwork if it means I get the most advanced scan on the planet in a facility that actually knows what it's doing!
Eric Mwiti
May 2, 2026 AT 23:59Oh sure, let's just trust the AI to tell us if we're dying. I'm sure it's totally foolproof and won't lead to more unnecessary biopsies. Brilliant.
James Harrison
May 3, 2026 AT 22:24It's a tough balance between knowing the truth and the peace of mind that comes with not knowing. Sometimes the burden of a 'probably benign' result is a weight one carries every day until the next scan.
Nila Sawyer
May 4, 2026 AT 10:26This is such a wonderful piece of information because it empowers us to take control of our health and honestly, seeing that 20% reduction in deaths is just so incredibly motivating for anyone who has been hesitant to visit the doctor! 🌟 It's all about longevity and loving ourselves enough to get checked even when we're scared, and I really hope everyone who qualifies takes this chance to breathe easier knowing they're proactive! ✨💖
Jaclyn Vo
May 5, 2026 AT 05:59Um, hello? Did anyone notice how the Medicare age cap is lower than the USPSTF? 🙄 Talk about a total mess! Why have two different numbers? It's literally such a headache for patients to figure out who's paying for what! 💅
suresh kumar
May 5, 2026 AT 14:41This is some spicy medical business right here! I bet the doctors are laughing their heads off seeing people panic over a tiny nodule that's probably just a bit of old lung gunk from a bad cold ten years ago. Just a wild ride through the doughnut machine!
Beena Garud
May 7, 2026 AT 00:45One must contemplate the ethical implications of overdiagnosis. The pursuit of absolute certainty often leads us to treat conditions that would never have manifested as a clinical problem, thus altering the natural course of a human life for a statistical phantom.
Jon Moss
May 7, 2026 AT 02:01I can see why the false positives are scary. It's a lot to handle mentally.
sachin singh
May 8, 2026 AT 23:29The integration of AI and the PLCOm2012 model seems like a very promising direction for personalized medicine. It would be most beneficial to move toward a risk-based approach rather than relying solely on chronological age and pack-years.
Michael Chukwuma
May 10, 2026 AT 14:22I really appreciate the way the Lung-RADS system is explained here. It makes the whole process feel much more structured and less like a guessing game for the patient.